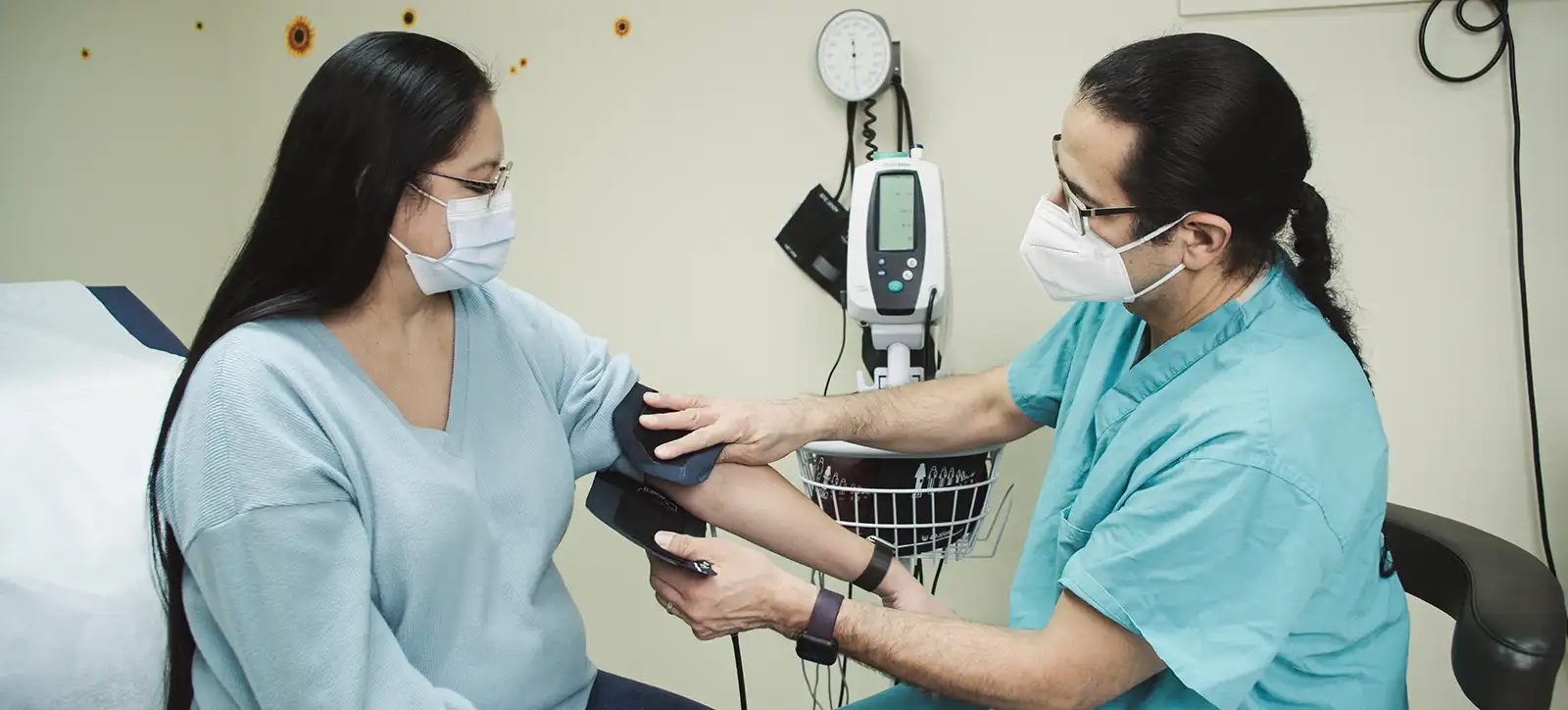
Prior to the 16th century and contact with European colonists, there were over 1,000 tribes comprised of nearly 60 million indigenous people living in North America. These were highly sophisticated cultures skilled in large-scale agriculture, adept at long-distance trading, and familiar with varying degrees of technological development. Though certain illnesses, diseases, and parasitic infections were present among these early populations, a traditional diet of food hunted and gathered from the land and low in fat, sugar, and sodium, as well as healthy socioeconomic environments, natural pharmacology, and a wealth of traditional healing practices, helped keep wide-spread health events at bay.
Rapid Dutch, French, and English colonization from 1534 to 1620, as well as the subsequent expansion of European settlers across the country, not only introduced new pathogens to AI/AN populations, they also put into motion cycles of destabilization among Native communities that would lay the groundwork for generations of mistrust in mainstream medical establishments, historical trauma, and persistent health disparities.
Epidemics defined the early post-Columbian health experiences of indigenous communities. Smallpox, for example, first swept across the North American continent in the late 1770s. Nearly every tribe was affected, but it hit especially hard in the Pacific Northwest. The disease resurged in 1837, decimating tribes in the northern Great Plains, then surfaced again in 1851. Other illnesses were quick to spread and impact AI/AN populations included measles, chickenpox, and influenza.
The era of eugenics soon followed, driven by the idea through limiting reproduction in certain populations would improve the population. Even as government programs were established to provide services, they still operated under the pervasive assumption that AI/AN people were mentally, morally, and socially defective, incapable of making their own health decisions. As late as the 1960s and 1970s, years after many state laws banned it, thousands of Native American women—somewhere between 25% and 50% of them—were subjected to forced sterilization by the Indian Health Services.
This turbulent history includes boarding schools and the forced removal of American Indian and Alaska Native (AI/AN) children from their families cultivated within indigenous populations a broad distrust of the government and modern medicine, further resulting in a host of health disparities in the collective health of Native communities. Burdened by higher rates of infant and neonatal mortality, chronic disease, mental illness, substance abuse, alcoholism, and suicide, AI/AN communities have a significantly lower life expectancy than white Americans. AI/AN populations are twice as likely to develop diabetes and nearly six times as likely to contract tuberculosis as the greater population and develop heart disease, cancer, lung disease along with higher rates of obesity. More recently, during the first year of the COVID-19 pandemic, AI/AN populations experienced the highest rates of infection, hospitalization, and death compared with any other ethnicity or race.
However, despite these challenges, indigenous populations have continued to persevere, pursuing and demanding the breadth and depth of health and medical services, as well as the quality of care, they rightly deserve.
Individual Efforts + Legal Advancements
Many individuals took it upon themselves to improve the conditions of their communities and tribes, defying boundaries of race, gender and socioeconomics.
In 1889, Susan La Flesche, a member of the Omaha tribe, became the first AI/AN woman to graduate from medical school. She returned to her home reservation as the only physician treating patients across 1,350 square miles. In 1913, she founded a hospital there and spent nearly 25 years treating patients and advocating for better health and hygiene practices.
Not long after, in 1892, Isabel Cobb, a Cherokee woman from Tennessee, earned her medical degree and became the first female physician in Indian Territory, the land established by the U.S. Government during the policy of Indian Removal. Holding degrees from the Cherokee Female Seminary and Glendale Female College, as well, Isabel was more educated than most women of her time, which she relied upon during her nearly 40 years treating patients and practicing medicine in the Cherokee Nation.
Other notable individuals include:
Susie Walking Bear Yellowtail, a member of the Crow nation, was one of the first Native American nurses in the U.S. She fought the policy of forced sterilization and helped reduce the language barriers keeping Native patients from quality care.
Carlos Montezuma, the first Native man to earn a medical degree, graduated from Chicago Medical College in 1889.
Dr. Patricia Nez Henderson, a member of the Navajo Nation whose research on genetic nicotine use in Native Americans has contributed to national smoking reduction efforts.Though far from perfect, federal legislation has helped pave the road for improvements in AI/AN healthcare. This work continues to evolve in scope, providing increasingly more protection, freedom, and provisions for Native tribes. Federal Legislation advancements include the Snyder Act of 1921, Public Law 93-638 (Indian Self-Determination and Education Assistance Act of 1975), Indian Health Care Improvement Act of 1976, Indian Gaming Regulatory Act of 1988 and more.
Tribes Take Charge
AI/AN healthcare systems operated by tribes often run more efficiently and more effectively and provide a higher quality of care when compared to non-tribal-led facilities. By focusing on building doctor-patient relationships and delivering healthcare designed to address the specific social and cultural issues facing AI/AN communities, tribal-led health systems can be proof that the best healthcare for AI/AN communities is provided by AI/AN healthcare professionals.
Cherokee Nation. The health care system operated by the Eastern Band of Cherokee Indians in Asheville, North Carolina, has dedicated its efforts to fighting opioid addiction within its community. It now includes one of the largest integrated mental health facilities in the state, a state-of-the-art $82 million facility paid for primarily from gambling revenue. The Cherokee Nation was ahead of the country and its state in getting its people tested and vaccinated during the early months of the COVID-19 pandemic.
Alaska Natives. Alaska Natives have developed an integrated culture-based care model called the Nuka System for Care that is tailor-made for tribal healthcare. By approaching a patient’s physical, mental, spiritual, and emotional health simultaneously, the Nuka System of Care provides a model more consistent with traditional healing, which does not separate different aspects of health. Patients are assigned a multi-disciplinary team that includes a primary care provider or nurse practitioner, a nutritionist, a pharmacist, and a behavioral health specialist for comprehensive care that treats the entire person.The Nation’s Only Tribally Affiliated Medical School. Oklahoma State University Center for Health Sciences and the Cherokee Nation have partnered together to establish the nation’s only tribally affiliated medical school. The medical school is located in the capital of the Cherokee Nation in Tahlequah, OK.
Work Left to Do
While many tribes are experiencing expansive new hope and opportunities for better healthcare, many more remain underserved, especially in locations where higher poverty, lack of resources, and geographic isolation make investment difficult, if not impossible.
For tribes on land far from urban areas that lack sufficient water, farmable land, or development opportunities, gaming offers help to bolster some of those economies, provide services and employment for citizens, and change the economic and social climates in and around the area. Where casinos or gaming may not be feasible or desired, philanthropy or partnerships with academic health systems may be necessary to fill the gaps in financing and funding.Telemedicine for communities in rural and underserved areas can help deliver timely care that would otherwise be unavailable, as can expanding the supply of providers allowed to practice in tribal areas to include physician assistants, nurse practitioners, and other non physician professionals.
AAIP and the Future of AI/AN Health
The COVID-19 pandemic has shed new light on an old reality, one that AI/AN populations have been coping with for generations-lack of infrastructure to cope with emerging disease outbreaks. However, as tribal nations begin to take the lead on how they serve their communities, better opportunities for reliable healthcare and preventative medicine are critical in creating trust in modern medical practices, practices that can help preserve and ensure the survival of native culture for our children. Vaccines such as influenza, COVID-19, and preventable childhood diseases are more readily adopted and accepted by populations who have taken time to develop trust, feel cared for, and respected by healthcare institutions that are invested in them and their futures.
To find out more about AAIP’s vaccine programs, visit us at wordpress-509372-3778584.cloudwaysapps.com.
